The Stem Cell Transplant and Cellular Immunotherapy program at MedStar Georgetown is the only program in the Washington, D.C., metropolitan area to offer chimeric antigen receptor (CAR) T-cell therapy for adults. CAR T-cell clinical trials are ongoing in the U.S. and commercially approved treatment is available.
Our Stem Cell Transplant and Cellular Immunotherapy program offers all FDA approved CAR T-Cell therapies (YESCARTA®, KYMRIAH®, TECARTUS™, ABECMA®, Breyanzi®, and Carvykti®) to treat certain types of blood disorders and cancers.
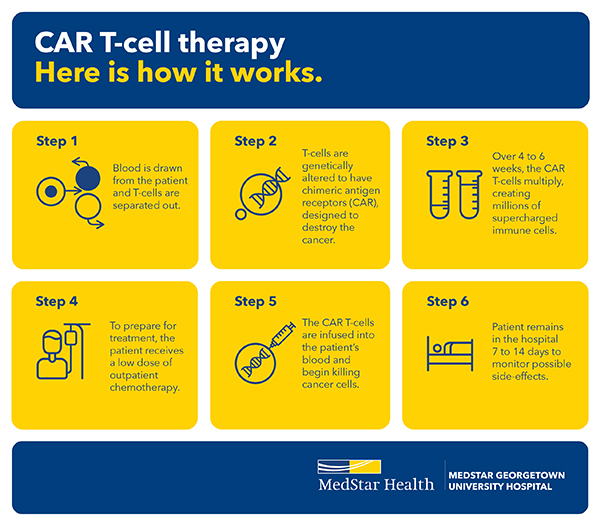
CAR T-cell therapy involves collecting immune cells from your blood, modifying them in a lab, and returning the modified cells to you via an IV infusion. The goal is to stimulate your immune system to more effectively target cancer cells and eliminate disease.
The U.S. Food and Drug Administration has approved CAR T-cell therapy to treat adult patients with certain types of B-Cell Lymphoma that have not responded to other therapies or who have relapsed after two other kinds of treatment.
Videos
What to expect during CAR T-cell therapy
Before treatment
At your first visit, you will meet with your care team to:
-
Determine if you are an appropriate candidate to receive CAR T-cell therapy
-
Discuss your treatment approach
-
Discuss the CAR T-cell therapy process, potential side effects, and outcomes
-
Understand the impact on your quality of life and day-to-day activities
CAR T-cell therapy begins with a process involving blood collection, to obtain immune cells needed for CAR T-cell manufacturing.
Your blood will be collected by an Apheresis machine. The machine will sort your T-cells from your blood. The non-T cells are returned to your body. This procedure can take up to six hours and is performed on an outpatient basis.
Your T cells are then sent to a lab to be genetically modified. The chimeric antigen receptor, or CAR, is attached to the T-cells. The CAR(s) grow and expand in the lab and are ready to be re-infused into your body in approximately three weeks.
During CAR-T cell therapy
- You will receive chemotherapy to prepare your body to receive the modified CAR T-cells. Your chemotherapy regimen may be given on an outpatient or inpatient basis.
- Your CAR T-cells will be infused back to you after receiving chemotherapy. You may be admitted to the hospital to receive CAR T-cell therapy.
After receiving CAR T-cell therapy, you will be closely monitored by your care team at MedStar Georgetown. Depending on the type of CAR T-cell therapy given, some patients may remain in the hospital for two weeks after their CAR T-cell infusion.
The biggest side effects of CAR T-cell therapy include the development of cytokine release syndrome (CRS) and neurotoxicities. CRS syndrome means that your body is setting up an immune response and substances called cytokines are released. Signs of CRS include lowered blood pressure, fever, rash, chills, and abnormal laboratory values. If patients experience severe side effects after CAR T-cell therapy, they may require care in an intensive care unit (ICU).
Neurotoxicity signs include dizziness, forgetfulness, and seizures. Some patients may experience difficulty in speaking or writing. Your doctor and clinical team will monitor you carefully for abnormal symptoms and signs of neurotoxicity.
After CAR T-cell treatment
Treatment does not end after CAR T-cell therapy. You will require monitoring over a period of years to ensure that your cancer does not come back.
You will still need to see your primary oncologist for regular monitoring and check-ups. You will continue to see your Cellular Immunotherapy care team at MedStar Georgetown.
Our location
Distance from Change locationEnter your location
MedStar Health: Stem Cell Transplant and Cellular Immunotherapy Program at MedStar Georgetown University Hospital
3800 Reservoir Rd., NW 2 East Main Building Washington, DC 20007
Awards and recognitions

Our program at MedStar Georgetown University Hospital has been awarded FACT Accreditation. Home to the nations’ largest stem cell collection facility, it’s the region’s only adult, Foundation for the Accreditation of Cellular Therapy (FACT)-accredited program for autologous transplant, allogeneic transplant, and cellular immunotherapy.
Our team
Our multidisciplinary team is dedicated to your care. Your team care includes:
- A dedicated nurse coordinator
- A dedicated social worker
- A cellular therapy physician
- Trained and experienced nursing staff
- Financial coordinator











