MedStar Georgetown’s First Living Donor Kidney Recipient Gets Second Transplant - 40 Years Later
Maryland Woman Celebrates Four Decades of Transplant Progress for Donors and Recipients
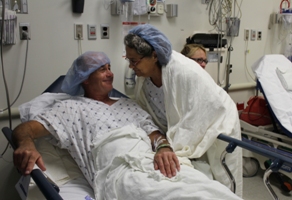
(Washington, D.C.,) Brenda Hudson’s transplanted kidney wasn’t supposed to function this long.
At the age of 12 in the 1970’s, then Brenda Robinson was diagnosed with lupus that slowly and steadily destroyed her kidneys and caused multiple life threatening health problems. Her face swelled from the massive doses of steroids that kept her alive. She survived a diabetic coma that lasted most of a summer. Brenda’s parents drove her from Upper Marlboro to Georgetown three times a week for exhausting dialysis treatments that were doing the work her kidneys no longer could. When Brenda was about 17 her physicians began to talk about kidney transplant.
“I just remember feeling so sick all the time,” said Brenda. “Kidney transplant was pretty new back then but I wasn’t afraid of it at all if it was going to make me feel better. I said ‘sign me up.’ ”
Testing showed that her 20 year old sister Michelle Robinson Tucker was as close a match possible without being identical twins. After careful preparation, on October 20, 1976 Brenda became the first person ever to receive a kidney transplant from a living donor at then Georgetown University Hospital.
“We expect a kidney from a living donor to last, on average, 15 to 18 years,” said Mathew Cooper, MD, director, Kidney and Pancreas Transplantation at the MedStar Georgetown Transplant Institute. “Forty years is spectacular.”
But in recent years, Brenda’s diabetes started affecting her health. She needed heart surgery in March of 2015 and had to start dialysis a year and a half ago as her transplant began to fail. Doctors told her she would need another kidney. The sooner, the better.
“I couldn’t imagine that I would get a second chance for a transplant,” said Brenda. But her husband Dana Hudson turned out to be a compatible donor. And in a surgery very different from the one she had 40 years ago, Brenda received a second kidney on June 28, 2016. In a carefully choreographed set of surgeries, Seyed Ghasemian, MD, laparoscopically removed one of Dana Hudson’s kidneys; Dr. Cooper then transplanted the kidney into Brenda Hudson.
Brenda, Michelle and Dana’s experiences with kidney transplant read like a “then and now” chapter in a medical text book and speak to the history of kidney transplantation at Georgetown - a lesson in how vastly transplant medicine and surgery have improved in the years since Brenda had her first kidney transplant.
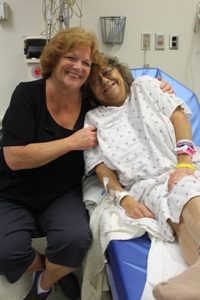
The method for Brenda’s transplant in 1976 involved a then standard two-stage process. The first step was the removal of her injured kidneys and her spleen requiring her to immediately begin dialysis treatments. About a month later she received her sister’s kidney in a surgery that lasted several hours.
Since Brenda was Georgetown’s first patient to receive a kidney from a living donor, she remembers having her own isolated wing of the hospital and her own nurse. She was carefully monitored in the hospital for a month.
“When my family came to visit me in the hospital after the transplant they had to dress in these big sterile gowns from head to toe and were so covered up that I couldn’t even recognize who was who,” Brenda recalled. The doctors and nurses were so afraid I was going to catch something to ruin my new kidney. And when I went home from the hospital I had to wear a mask in public for six months. “
“Clinicians were much more heavy handed back then with immunosuppression in those early days,” said Dr. Cooper. “The drugs Brenda would have received were not as targeted as they are now. Today our medications prevent rejection better and have fewer side effects. And our recipients usually go home in about four days.”
“The other nice thing is that today living donors are much more able to see the benefit of their donation. In the old days they might have been taken aback at how uncomfortable they were following surgery,” said Dr. Cooper.
Brenda’s sister Michelle remembers what is was like to donate her kidney back in 1976. She proudly shows off the large scar that stretches about 12 inches from the midline of her abdomen all the way under her right ribcage.
“I would do this all over again for my sister,” said Michelle. “But it was a big surgery as I look back on it. I was in the hospital with some complications for about a month and it took me almost a full year to feel back to normal.”
Dr. Cooper says the old way to remove a kidney from a living donor was to start an incision at the bottom of the rib cage and split the muscles sometimes requiring removing a lower rib to get to the organ, which was painful. Patients were usually in the hospital for 10 days and confined to the home for three to four weeks.
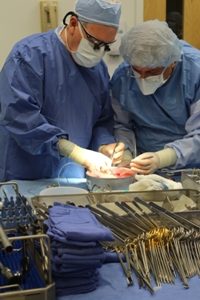
Transplant surgeons needed only four 5mm-1cm incisions to remove Dana’s kidney laparoscopically. He went home two days following surgery.
“I was happy to do this for my wife,” said Dana Hudson. “I just couldn’t watch Brenda be so sick and so debilitated by dialysis.”
“It’s amazing what Dana has done for me. He’s a keeper,” Brenda laughs. “And all these people who donate kidneys are truly special people.”
“Of our approximately 220 kidney transplant we perform each year, 25-30 percent of them come from living donors,” said Jennifer Verbesey, MD, Director of the Living Donor Kidney Transplant Program at the MGTI. “Contrasting to a time when Brenda was the only patient on her wing of the hospital after her transplant in 1976, at the time of her surgery this time, our transplant teams performed six living donor transplants in 36 hours. Some of those happened as a result of MGTI’s Paired Kidney Exchange (PKE) Program in which willing, eligible yet incompatible donor and recipient pairs exchange donors thus allowing both recipients to experience the benefits of living donor transplantation. That’s quite a change in the approach to transplant in 40 years.”
“I’m so thankful for how good I feel all day long,” Brenda said about a week after her transplant. “No more lethargy, nausea, cramping that I felt from dialysis and not have to deal with that anymore is just so unbelievable. And I feel positively wonderful.”
With the help of tutors, Brenda went on to graduate with her class in 1977 from Frederick Douglas High School in Upper Marlboro, Maryland. She then completed a four year degree in food and nutrition at University of Maryland College Park.
After her first transplant Brenda’s physicians advised that she should never become pregnant. Doctors couldn’t predict the stress that carrying a child to term would place on a kidney and what complications her anti-rejection medications would cause to her unborn baby.
“But I was a pioneer there too. I guess I didn’t really listen because ten years after my transplant I gave birth to my miracle baby Bradley and I had him at Georgetown. He’s now 30, big and strong and has always been just fine.”
When asked to compare her two transplant experiences that span 40 years, Brenda laughed. “This one was a lot easier in every way. Mostly, I feel so much better getting this kidney from someone knowing that he didn’t have to go through what my sister went through 40 years ago. There really is no comparison. What hasn’t changed is the wonderful expertise and compassionate TLC I received from all the people at Georgetown, both then and now. ”
Categories
Media Contact
Marianne Worley
Director of Media Relations
703-558-1287202-405-2824
worleym@gunet.georgetown.edu









